HPV / Genital Warts

Contents
What is HPV / Genital Warts?
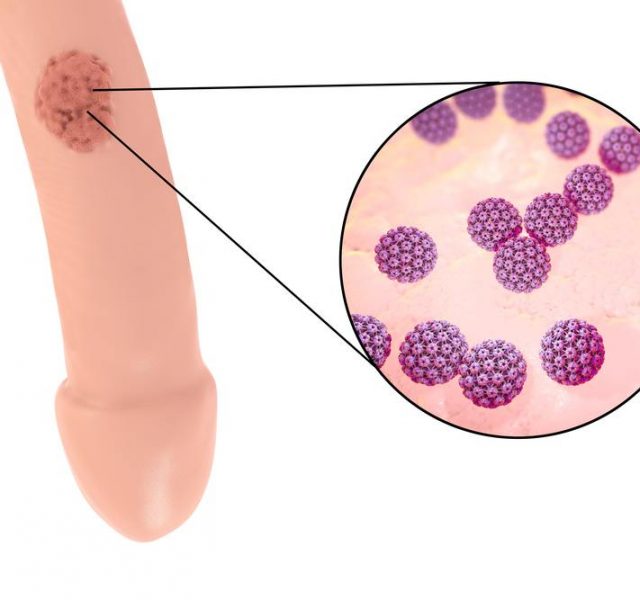
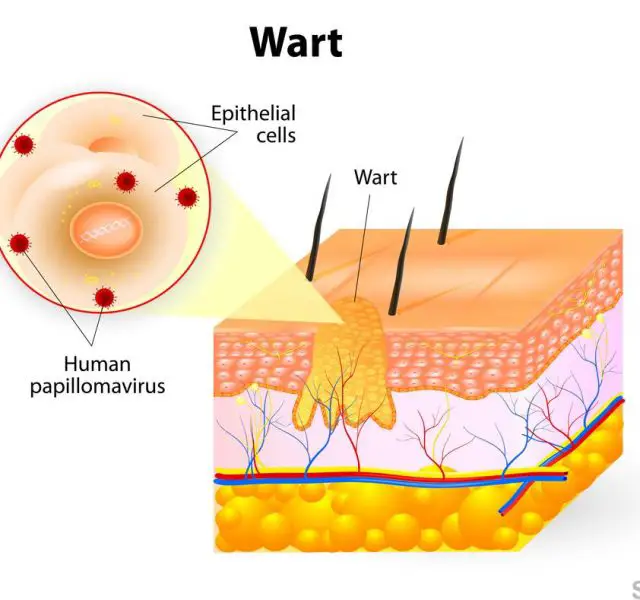
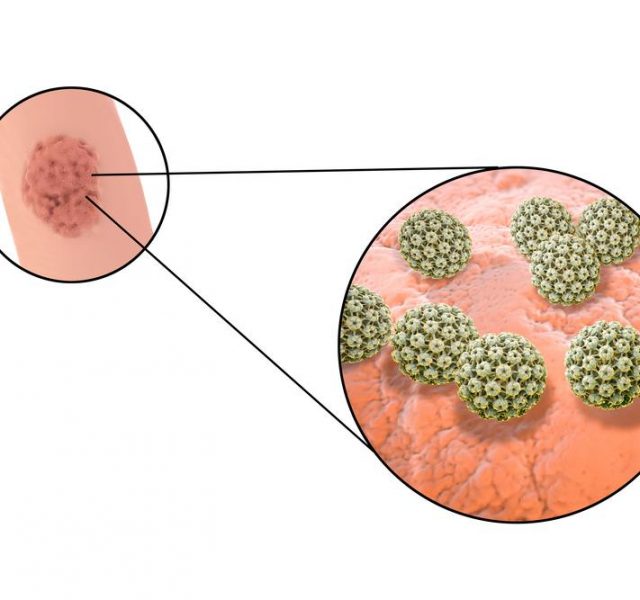
Human Papilloma Virus (HPV) — a group of more than 70 viruses, some of which can lead to cervical cancer. Several strains of HPV cause external genital warts.
How is it contracted?
Through oral, anal, and vaginal sex and through skin-to-skin contact. To help prevent infection, use a condom. It’s not clear exactly how effective condoms are at protecting against HPV and genital warts, but they will protect you against other STDs, including HIV.
Incubation Period
Anywhere from one month to several years.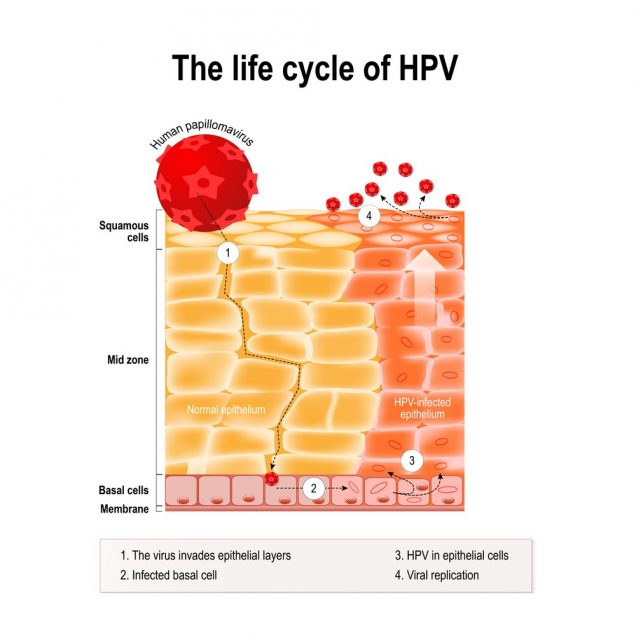
Signs and Symptoms of HPV / Genital Warts
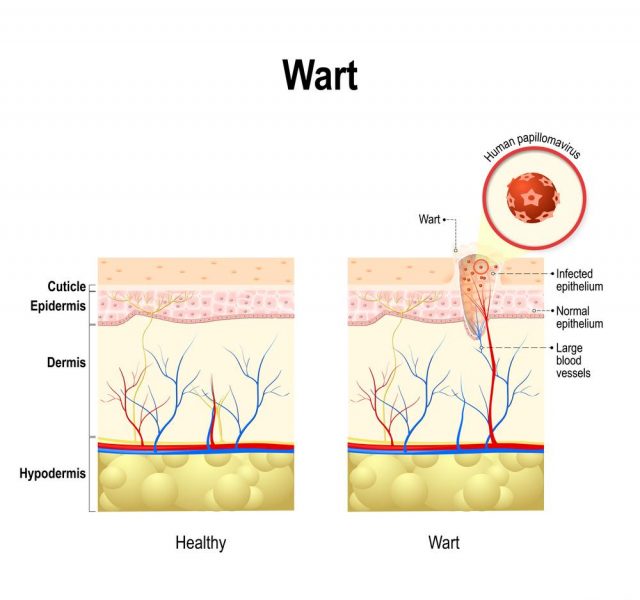
Many types of HPV have no symptoms, though some cause visible genital warts that may be found in the vagina or urethra or on the cervix, vulva, penis, or anus. Rarely, they are found in the mouth or throat. Warts are often flesh-colored, soft to the touch, and may look like miniature cauliflower florets. They usually grow in more than one area and are often painless, although they may itch.
Testing
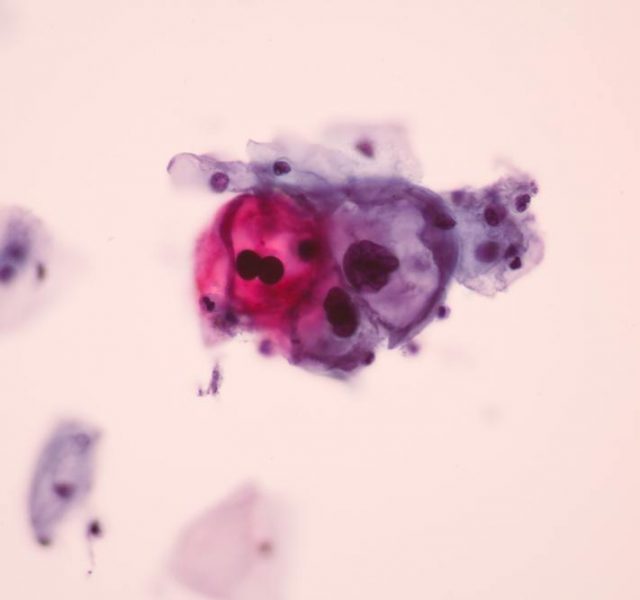
Once a woman becomes sexually active, or by age 18, she should get an annual Pap smear to detect any abnormal changes in the cervix. Pap smears are the first line of defense against the HPV family of viruses, which is typically without symptoms.
If your Pap test comes back abnormal, your doctor will likely order a second one to confirm the results. A cervical DNA swab test can also be performed to identify which specific HPV virus you have (only a few types of HPV have been linked to cervical cancer and these are usually not the ones that cause genital warts). If HPV is found, a colposcopy — a test that examines the tissues of the vagina and cervix using a magnifying lens — is usually ordered.
Treatment of HPV. Is there cure for it?
There is no cure for HPV, so treatment aims at controlling outbreaks of warts — if you have a strain that causes visible warts. If a woman is diagnosed with certain strains of HPV, her doctor may suggest a biopsy of cervical tissue to check for signs of cancer. It is important to note that many women with HPV do not get cervical cancer, but HPV infection is an important risk factor for the disease. Further treatment varies widely depending on what your doctor learns from a colposcopy, DNA testing, and/or a biopsy of cervical tissue.
To treat visible genital warts, there are several chemicals that can be directly applied. Some are prescribed for use at home, others may cause discomfort and must only be used under a doctor’s supervision, and some may not be used during pregnancy. Genital warts also may be removed using cryotherapy (freezing), burned off with electrocauterization, or removed with surgery or lasers. In at least 30 percent of treated cases, the warts grow back again.
If you are not treated
Since there are strains of HPV that are linked to cervical cancer, failing to seek treatment can be fatal. But since many types of HPV are basically harmless, they need only be monitored with yearly Pap smears (or more frequently — every three to six months — if a result comes back abnormal).If genital warts are allowed to grow without treatment, they can block the vagina, urethra, or anus, and become very uncomfortable.
Depending on where they are on the body, genital warts can cause sores and bleeding. An increase in the size and number of the warts is also more likely during pregnancy and when a person’s immune system is compromised by diabetes, an organ transplant, Hodgkin’s disease, or HIV/AIDS, among other conditions.